Understanding Septal Infarct: Causes, Symptoms, Diagnosis, and Treatment
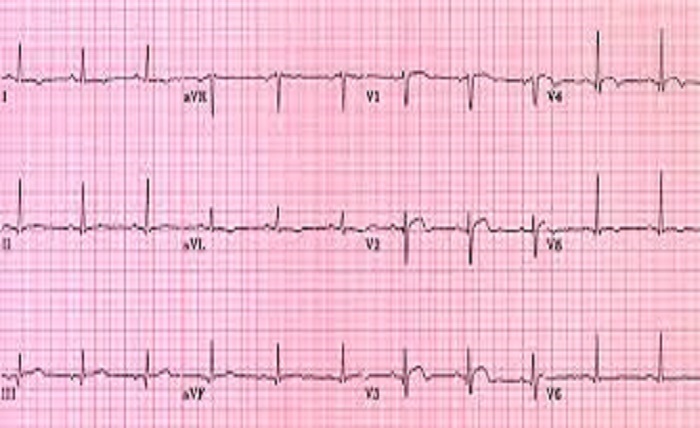
Septal infarct refers to a specific type of heart attack that occurs in the septum, which is the wall that divides the left and right sides of the heart. This condition can have significant implications for a person’s cardiac health and requires prompt medical attention. In this article, we will delve into the causes, symptoms, diagnosis, and treatment options for septal infarct.
What is Septal Infarct?
Septal infarct is a myocardial infarction that affects the septum, a crucial part of the heart. The septum is responsible for separating the left and right chambers of the heart, namely the left and right ventricles. When a blockage occurs in the coronary arteries that supply blood to the septum, it can lead to inadequate blood flow and oxygen delivery, resulting in tissue damage or death in that area. This is known as septal infarct or septal myocardial infarction.
Causes of Septal Infarct:
Septal infarct usually occurs as a consequence of coronary artery disease (CAD). CAD develops when plaque, a buildup of cholesterol, fatty deposits, and other substances, narrows the coronary arteries. This narrowing restricts blood flow and increases the risk of blood clots, leading to a heart attack. The risk factors for septal infarct include smoking, high blood pressure, high cholesterol levels, obesity, diabetes, and a family history of heart disease.
Symptoms of Septal Infarct:
The symptoms of septal infarct can vary from person to person. However, some common signs to watch out for include chest pain or discomfort, shortness of breath, fatigue, dizziness, nausea, and vomiting. It is important to note that some individuals may not experience any symptoms at all, which is known as a silent heart attack. Regardless, if you experience any of these symptoms, it is crucial to seek immediate medical attention.
Diagnosing Septal Infarct:
To diagnose septal infarct, a healthcare provider will perform a thorough evaluation, which may include a review of medical history, physical examination, and several diagnostic tests. These tests may involve an electrocardiogram (ECG) to assess electrical activity in the heart, blood tests to measure cardiac enzymes and biomarkers, and imaging tests such as an echocardiogram, cardiac MRI, or coronary angiography to evaluate the structure and function of the heart and its blood vessels.
Treatment Options for Septal Infarct:
The treatment for septal infarct aims to restore blood flow to the affected area, relieve symptoms, prevent complications, and reduce the risk of future cardiac events. The specific treatment plan may vary depending on the severity of the condition and individual patient factors. Immediate interventions may include medications like aspirin, beta-blockers, and nitroglycerin to manage pain and improve blood flow. In some cases, emergency procedures like angioplasty and stenting or coronary artery bypass surgery may be necessary to restore blood flow to the heart.
Post-Treatment Care and Lifestyle Modifications:
After experiencing a septal infarct, it is essential to make necessary lifestyle changes to promote heart health and reduce the risk of future cardiac events. This may involve adopting a heart-healthy diet rich in fruits, vegetables, whole grains, and lean proteins, regular exercise, maintaining a healthy weight, quitting smoking, managing stress, and effectively controlling underlying medical conditions such as hypertension and diabetes. Following the prescribed medication regimen and attending regular follow-up appointments with a healthcare provider are also crucial.
Conclusion:
Septal infarct is a serious condition that requires prompt medical attention. Understanding its causes, recognizing its symptoms, and seeking timely diagnosis and treatment are vital for improving outcomes and reducing the risk of complications. By making necessary lifestyle modifications and adhering to the prescribed treatment plan, individuals can take proactive steps towards maintaining a healthy heart and overall well-being.